Expo
view channel
view channel
view channel
view channel
view channel
view channel
view channel
RadiographyMRIUltrasoundNuclear MedicineGeneral/Advanced ImagingImaging IT
Events

- AI Tool Predicts Breast Cancer Risk Years Ahead Using Routine Mammograms
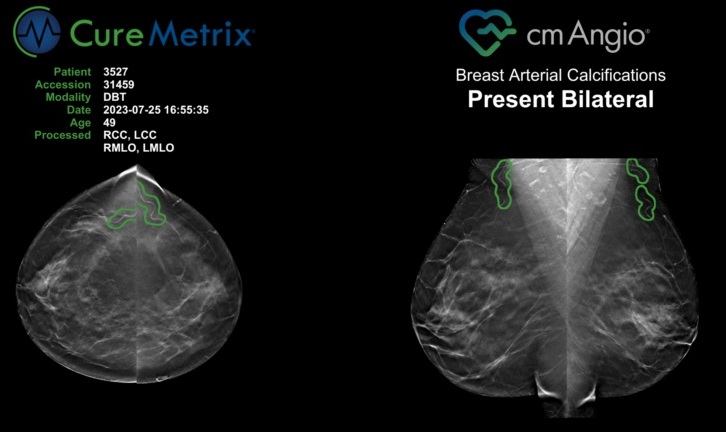
- Routine Mammograms Could Predict Future Cardiovascular Disease in Women
- AI Detects Early Signs of Aging from Chest X-Rays
- X-Ray Breakthrough Captures Three Image-Contrast Types in Single Shot
- AI Generates Future Knee X-Rays to Predict Osteoarthritis Progression Risk
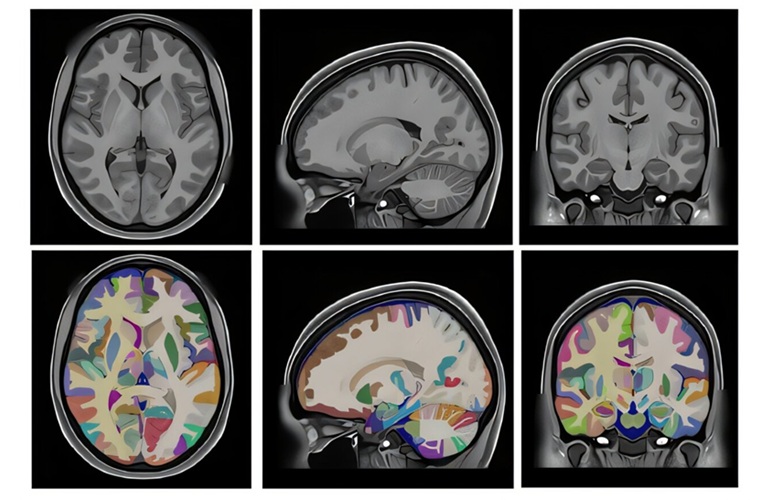
- Ultra-Detailed Brain Atlas Enhances Early Detection of Neurological Disorders
- Study Finds Advanced Imaging Significantly Reduces Unnecessary Prostate Biopsies
- New Material Boosts MRI Image Quality
- AI Model Reads and Diagnoses Brain MRI in Seconds
- MRI Scan Breakthrough to Help Avoid Risky Invasive Tests for Heart Patients
- New Imaging Tool Sheds Light on Tumor Fat Metabolism
- Radiopharmaceutical Molecule Marker to Improve Choice of Bladder Cancer Therapies
- Cancer “Flashlight” Shows Who Can Benefit from Targeted Treatments
- PET Imaging of Inflammation Predicts Recovery and Guides Therapy After Heart Attack
- Radiotheranostic Approach Detects, Kills and Reprograms Aggressive Cancers
- Groundbreaking Technology to Enhance Precision in Emergency and Critical Care
- Reusable Gel Pad Made from Tamarind Seed Could Transform Ultrasound Examinations
- AI Model Accurately Detects Placenta Accreta in Pregnancy Before Delivery
- Portable Ultrasound Sensor to Enable Earlier Breast Cancer Detection
- Portable Imaging Scanner to Diagnose Lymphatic Disease in Real Time
- AI Tool Offers Prognosis for Patients with Head and Neck Cancer
- New 3D Imaging System Addresses MRI, CT and Ultrasound Limitations
- AI-Based Tool Predicts Future Cardiovascular Events in Angina Patients
- AI-Based Tool Accelerates Detection of Kidney Cancer
- New Algorithm Dramatically Speeds Up Stroke Detection Scans
- Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
- AI-Based Mammography Triage Software Helps Dramatically Improve Interpretation Process
- Artificial Intelligence (AI) Program Accurately Predicts Lung Cancer Risk from CT Images
- Image Management Platform Streamlines Treatment Plans
- AI Technology for Detecting Breast Cancer Receives CE Mark Approval
- GE HealthCare and NVIDIA Collaboration to Reimagine Diagnostic Imaging
- Patient-Specific 3D-Printed Phantoms Transform CT Imaging
- Siemens and Sectra Collaborate on Enhancing Radiology Workflows
- Bracco Diagnostics and ColoWatch Partner to Expand Availability CRC Screening Tests Using Virtual Colonoscopy
- Mindray Partners with TeleRay to Streamline Ultrasound Delivery

 Expo
Expo
- AI Tool Predicts Breast Cancer Risk Years Ahead Using Routine Mammograms
- Routine Mammograms Could Predict Future Cardiovascular Disease in Women
- AI Detects Early Signs of Aging from Chest X-Rays
- X-Ray Breakthrough Captures Three Image-Contrast Types in Single Shot
- AI Generates Future Knee X-Rays to Predict Osteoarthritis Progression Risk
- Ultra-Detailed Brain Atlas Enhances Early Detection of Neurological Disorders
- Study Finds Advanced Imaging Significantly Reduces Unnecessary Prostate Biopsies
- New Material Boosts MRI Image Quality
- AI Model Reads and Diagnoses Brain MRI in Seconds
- MRI Scan Breakthrough to Help Avoid Risky Invasive Tests for Heart Patients
- New Imaging Tool Sheds Light on Tumor Fat Metabolism
- Radiopharmaceutical Molecule Marker to Improve Choice of Bladder Cancer Therapies
- Cancer “Flashlight” Shows Who Can Benefit from Targeted Treatments
- PET Imaging of Inflammation Predicts Recovery and Guides Therapy After Heart Attack
- Radiotheranostic Approach Detects, Kills and Reprograms Aggressive Cancers
- Groundbreaking Technology to Enhance Precision in Emergency and Critical Care
- Reusable Gel Pad Made from Tamarind Seed Could Transform Ultrasound Examinations
- AI Model Accurately Detects Placenta Accreta in Pregnancy Before Delivery
- Portable Ultrasound Sensor to Enable Earlier Breast Cancer Detection
- Portable Imaging Scanner to Diagnose Lymphatic Disease in Real Time
- AI Tool Offers Prognosis for Patients with Head and Neck Cancer
- New 3D Imaging System Addresses MRI, CT and Ultrasound Limitations
- AI-Based Tool Predicts Future Cardiovascular Events in Angina Patients
- AI-Based Tool Accelerates Detection of Kidney Cancer
- New Algorithm Dramatically Speeds Up Stroke Detection Scans
- Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
- AI-Based Mammography Triage Software Helps Dramatically Improve Interpretation Process
- Artificial Intelligence (AI) Program Accurately Predicts Lung Cancer Risk from CT Images
- Image Management Platform Streamlines Treatment Plans
- AI Technology for Detecting Breast Cancer Receives CE Mark Approval
- GE HealthCare and NVIDIA Collaboration to Reimagine Diagnostic Imaging
- Patient-Specific 3D-Printed Phantoms Transform CT Imaging
- Siemens and Sectra Collaborate on Enhancing Radiology Workflows
- Bracco Diagnostics and ColoWatch Partner to Expand Availability CRC Screening Tests Using Virtual Colonoscopy
- Mindray Partners with TeleRay to Streamline Ultrasound Delivery